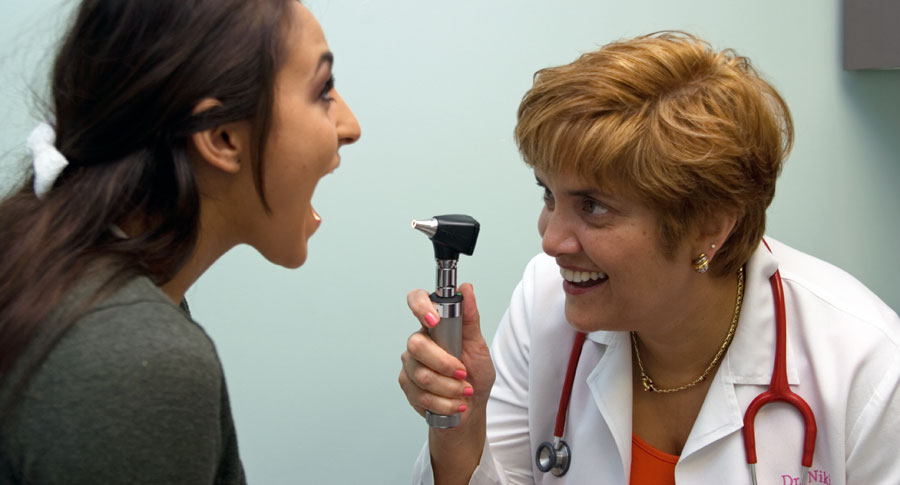Not long ago, the physicians at Pediatric Wellness Group (PWG) noticed a tip in the balance of its patient mix. Many of their newborns and diaper-clad tots were morphing into teens with a range of behavior-related health issues and young adults on the verge of leaving home.
College-age patients clamored to stay with the practice, fearing the pokings and proddings of a new clinician. There were patients with chronic illnesses who were aging out, facing an uncertain future with new specialists. And pediatricians found themselves just plain busier, treating patients who were neither big children nor little adults, but somewhere in between.
So, in turning its attention to this growing adolescent population, the San Francisco Bay-area practice pondered how to best serve a group of patients whose physical, behavioral and emotional needs are its most diverse and challenging.
“Our ultimate goal is to get better patient engagement among our adolescent population and give them tools to manage their own health.”Dr. Niki Saxena
Their solution? Create a separate clinic — one that treats adolescents as a distinct patient population, yet maintains PWG’s core medical home model emphasis on preventive health and education. Located down the hall from its pediatric offices in Redwood City, the planned Young Generation Wellness Group is scheduled to open in summer 2016.
“As a Patient-Centered Medical Home, our ultimate goal is to get better patient engagement among our adolescent population and give them tools to manage their own health,” says Dr. Niki Saxena, who manages PWG with partner Dr. Eileen Chan. “To achieve this, we think it’s helpful to physically separate out the adolescent piece. This reinforces the fact that there are different issues you’re dealing with, and sets up a different experience for the adolescent.”
PWG’s growing adolescent population is representative of pediatric practices across the country that are seeing a similar patient mix. Adolescents ages 12 through 21 make up one-third of the patient population in practices, according to a 2009 study by The National Alliance To Advance Adolescent Health.
Yet the field of adolescent medicine remains something of an anomaly among pediatric specialties. The job is demanding, time-consuming and often poorly paid — making it difficult for practices to invest in the array of services needed to improve health outcomes and prevent chronic conditions from continuing into adulthood.
The Right Location
Drs. Saxena and Chan’s practice, as well as others in cities near major teaching hospitals, are more immune to the economic barriers of opening an adolescent clinic. PWG is located at the mid-point of the San Francisco Peninsula, an area in the center of a booming high-tech industry.
“When we opened in 2011, we knew there was additional space if we wanted to expand, so that made it easy,” Dr. Saxena says. “Our community is going through a tremendous amount of growth that includes a huge influx of people and an expanding workforce.”
Recruiting physicians for PWG’s adolescent center is also comparatively easy, with its proximity to Stanford Children’s Center and University of California at San Francisco (UCSF). But the partners at PWG — a Level 3 Patient-Centered Medical Home — are choosy, interested in only those candidates whose values match theirs.
“Sometimes it’s less about titles and more about fit,” says Dr. Saxena.
Finding funding for a stand-alone practice was a different story. With a booming economy comes the high cost of doing business. Pay scales are higher and rent is exorbitant.
“Start-up cost is two- to three-times what anyone else would have, and most people can buy a building outright for what we pay in rent,” says Dr. Saxena. “It was hard work finding the type of funding that would work out for our practice. It was necessary for us to get creative and think outside the box.”
Dr. Saxena says practices should consider several sources — other doctors, banks, hospitals and lending institutions — when looking to expand their services and facilities.
“It’s worth having conversations and potentially partnering with multiple folks,” Dr. Saxena says. “Get your business program together and do your homework.”
Homework for PWG involved hiring a consultant with experience in start-up practices. The partners chose The Verden Group, a health care consulting firm based in Nyack, N.Y.
“In creating a business plan,” said Susanne Madden, Verden’s founder and CEO, “stakeholders looked at adolescent-focused services that are already available in the area. They found many existing services target teens and young adults who are already in trouble, leaving a gap for PWG to provide guidance and services that can prevent and educate against crisis situations.”
“The goal is to take the existing medical home model with PWG, replicate it, then apply it in treating a different population,” Madden says. “It will exist as a stand-alone practice which will be highly specialized and will make a very strong brand.”
Dr. Niki Saxena
PWG’s adolescent practice will serve patients ages 16 to 26. Many will be existing patients who have technically aged out of PWG; others may be young adults from other pediatric practices who have also aged out and are looking for specialized care for their stage of life. Still other patients may be teenagers who feel out of place in a pediatric setting. The day-to-day practice will be staffed by a family practitioner, an internist and a mental health worker.
“In our experience, there is a growing chunk of kids who don’t want to leave because they love the personalized care,” Dr. Saxena says. “Also, it’s great to offer the kids who age out an option we’ve vetted, as opposed to an office that may or may not share the same medical home model.”
Dr. Saxena’s partner, pediatrician Eileen Chan, says some 50 percent of her patients are now in their mid- to latter teens or are young adults. And the majority of her oldest patients don’t want to leave the practice, she says.
“They’re bonded to me and I’m bonded to them,” says Dr. Chan. “They don’t care if their doctor is a female or a male. They just want to have a relationship with a person they’ve trusted for a long time.”
Adds Dr. Chan: “It’s incredible to be able to have that gift with somebody who is comfortable telling you ‘I took this drug,’ or ‘I had unprotected sex,’ and then to whom I can say, ‘that wasn’t a good idea. Why would you do that?’”
Like most pediatric office common spaces, the waiting room at PWG is a lesson in bright primary colors. Kid-sized chairs are tucked under a kid-sized table. Patients waiting for their turn in the exam room can flip through picture books, or play with a toy in which red, yellow and blue marbles are pushed or pulled along a looping strand of wire.
PWG’s adolescent waiting room will be decidedly different — smaller and more intimate, as teenagers often feel more vulnerable in large, open spaces, said Dr. Saxena.
According to the American Academy of Pediatrics, a welcoming, teen-friendly environment may include adolescent-specific posters, or pamphlets on substance use and mental and sexual health.
Also, brochures on sensitive topics should be available in the examination rooms, and displaying information about the practice’s confidentiality policy and waiting times is key.
Dr. Saxena advises those looking to start an adolescent practice to do their homework.
“Do your market research, and don’t be afraid to think outside the box.”